What is Inflammation?
Inflammation. A word you may have heard associated with different chronic diseases, including heart disease. But what does inflammation mean? How does it relate to your heart health? How do you incorporate more anti-inflammatory foods into your meals to help prevent or mitigate chronic inflammation?
Let’s begin by defining and gaining an understanding of two different types of inflammation. In the short-term, inflammation is a life saving necessity. It protects us from infections and helps our bodies heal from injuries. Problems begin to develop when inflammation is present continuously throughout the body. When it has no direct and short-term purpose to address infections and heal the body. Let’s take a slightly deeper dive into the different types of inflammation.
Acute Inflammation
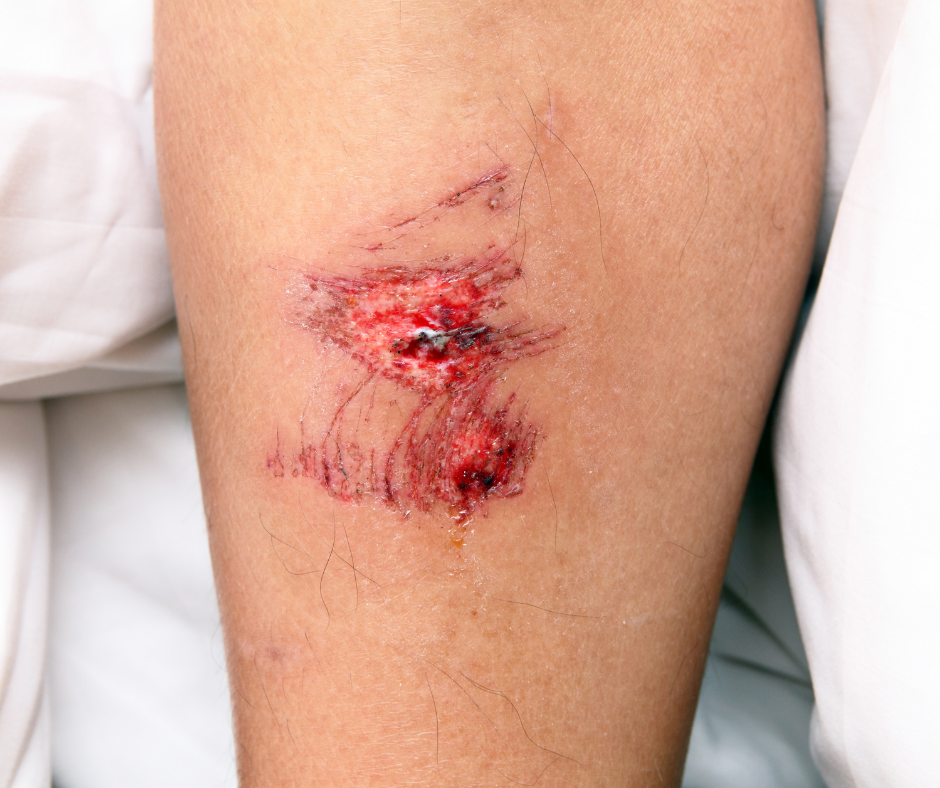
In general, acute inflammation goes away after the damage is healed, often within days or even hours. Acute inflammation is the “good” kind of inflammation because it does an essential job and then quiets itself down.
Acute inflammation is a healthy, self-limiting response to infections (sore throat) and injuries (cut, sprained ankle) in a centralized location. It is a natural and essential process that your body uses to defend itself against invading germs and heal injured cells and tissues. Your immune system produces specific biochemicals that can destroy invaders like bacteria and viruses, increases blood flow to areas that need it and cleans up debris. Proper healing and injury repair produces the painful, red, hot, swollen symptoms associated with acute inflammation.
Chronic Inflammation
When our immune system is repeatedly challenged and unsupported, inflammation may become chronic. Chronic inflammation is an unhealthy, self-perpetuating response at the root of many chronic conditions including cardiovascular disease, diabetes and cancer. This type of inflammation can exist throughout your whole body at lower levels. The symptoms are not localized to one particular area, appear gradually and last much longer – months or even years. This is the “bad” kind of inflammation.
Chronic inflammation is often invisible without immediate or serious symptoms, but over the long-term it’s been linked to many chronic diseases such as:

- Acne, eczema, and psoriasis
- Allergies and asthma
- Autoimmune diseases (arthritis, type 1 diabetes, multiple sclerosis, lupus)
- Cancer
- Chronic pain
- Gastrointestinal disorders (Crohn’s disease, ulcerative colitis)
- Heart disease and stroke
- High blood pressure
- Lung diseases (emphysema)
- Mental illnesses (anxiety, depression)
- Metabolic diseases (type 2 diabetes)
- Neurodegenerative diseases (Alzheimer’s, Parkinson’s)
How does chronic inflammation begin? It may start acutely—from an infection or injury—and then instead of shutting off, it becomes persistent. Chronic low-grade inflammation can also occur with exposure to chemicals (e.g., tobacco) or radiation, consuming an unhealthy diet or too much alcohol, not being very physically active, feeling stressed or socially isolated, and having excess weight.
Links Between Chronic Inflammation and Heart Disease and High Blood Pressure
Chronic inflammation may eventually lead to the destruction of the body’s normal and healthy cells, including the endothelial cells of the arterial wall. Endothelial cells play a key role in protecting us from heart disease (Houston, 2023) and high blood pressure. When endothelial cells lose their functionality, it is often referred to as endothelial dysfunction and can be detrimental in maintaining our heart health.
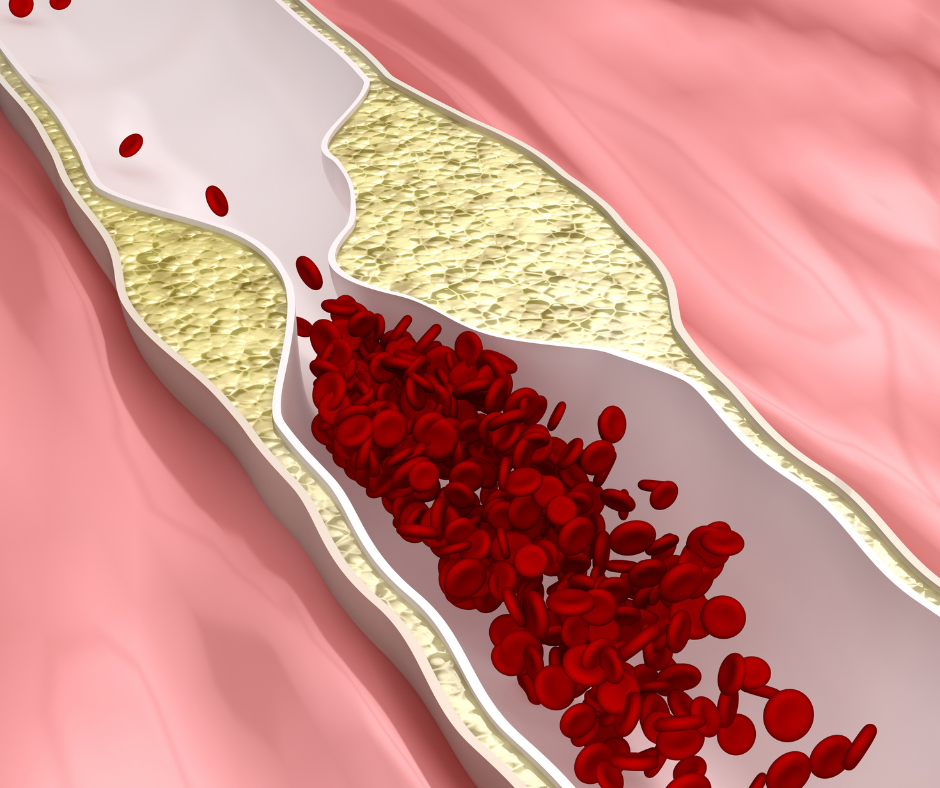
The compromised arterial wall is susceptible to substances accumulating beneath its surface or within the arterial wall. These substances do not belong beneath or within the arterial wall and further exacerbate the inflammatory immune response. The substances continue to build and may eventually form plaque. As plaque growth progresses, it usually expands beyond the arterial wall and begins to narrow the arteries and impede the flow of blood creating atherosclerosis. The artery wall becomes irritated by the plaque and may result in arteriosclerosis or “hardening of the arteries”.
Arterial plaque and stiffening of the arteries are underlying mechanisms of heart disease (Li, et al., 2018). Understanding the development of atherosclerosis has “implicated inflammation as a central contributor to the initiation and progression” of heart disease (Li, et al., 2018).
Endothelial dysfunction can also lead to the endothelium losing its ability to make substances to regulate blood pressure (Houston & Bell, 2021). Blood pressure can also be increased when the arteries lose their elastic stretch and become stiff and hardened as in the case of arteriosclerosis (Houston & Bell, 2021).
Anti-Inflammatory Foods
Food and lifestyle changes help to prevent and mitigate chronic inflammation.

Our eating patterns of today often lead us towards the path of chronic inflammation. Overly processed foods. Prevalence of fast food. Focus on convenience.
Anti-inflammatory foods include vegetables, fruits, whole grains, healthy fats and plant-based proteins. These are the foods that are often deficient within our meals.
While you may be familiar with anti-inflammatory foods, learning how to incorporate them into your meals is often the missing piece. Not anymore. Within the Heart Health Nutrition Program https://aknutrition.net/heart-health-nutrition-program, you learn how to slowly and gradually incorporate these foods so that they become second nature and a part of life moving forward.
Additional Anti-Inflammatory Lifestyle Behaviors
In addition to addressing inflammation through the power of food, here are some other lifestyle behaviors to implement over time. Remember, gradual change equates to sustainable change.
Be physically active

- Move more and sit less
- 150-300 minutes of moderately-intense (brisk walking) -OR- 75 minutes to 150 minutes of vigorously-intense (running) -OR- combination of moderately and vigorously-intense aerobic activity each week
- In addition, muscle-strengthening exercises of moderate or greater intensity involving all major muscle groups 2 or more days per week
- For more details visit https://health.gov/our-work/nutrition-physical-activity/physical-activity-guidelines/current-guidelines
Quit smoking and limit alcohol
- Quitting smoking can help reduce inflammation and several other health concerns by reducing exposure to toxins that are directly linked to inflammation
- Limit your alcohol intake to no more than one or two drinks per day

Restful sleep
- Disrupted sleep has recently been linked to increased inflammation and atherosclerosis so aim for 7-9 hours of restful sleep every night to help the body heal and repair
- Tips for better sleep: try to maintain a regular sleep-wake schedule every day, get exposure to natural daylight earlier in the day, avoid caffeine later in the day, cut out screen time an hour before bedtime and create a relaxing nighttime routine
Manage your stress
- Eliminate stress, where possible. Manage your stress via stress-reducing activities that you enjoy. Deep breathing, yoga, meditation, experiencing nature, reading a book, meaningful conversations with loved ones, belly-aching laugh, etc.
Socialize and connect with others
- Social isolation is linked with higher levels of inflammation, so reach out to family and friends (or make new ones)
See your doctor and dentist regularly

- Develop a relationship with your doctor. Visit them regularly. Get the standard blood tests annually and look at the results. Even though you may be in the “normal range” for some, or all, of your blood work, metrics may be gradually approaching out of range. Get on top of it now! Why wait? Inquire about how to prevent continued movement towards the abnormal and unhealthy levels.
- Request and inquire about additional blood test to measure inflammation due to its role in heart disease and high blood pressure.
- Some research suggests a connection between heart disease and inflammation caused by oral bacteria. Visit your dentist for regular cleanings.
